Pelvic Floor Specialist
Pelvic floor physiotherapists help women rehabilitate their pelvic floor region. The muscle groups within the core and pelvic region can be weakened by childbirth, surgery, genetics, heavy lifting, rapid weight gain, constipation, menopause, improper breathing mechanics, and more. These muscle groups aid in supporting the uterus, bladder, and bowels. They form a slinglike grouping from the pubic bone to the front of the tailbone at the back. Damaged or weakened pelvic floors can affect bladder and bowel control, leading to urinary and rectal incontinence or even pelvic organ prolapse.
At times, the pelvic floor can become overactive or hypertonic. This means that their pelvic floor muscles are overly tight and tense all of the time, even when they should be relaxed. Learning to relax and release the pelvic floor muscles (muscles contractions like the short contraction of the bulging of a bicep or long contraction, like the slow, contained stretching out of a bicep) will help ease overactivity. An overactive pelvic floor can cause many symptoms such as: back pain, pain during sex, heaviness or incontinence.
What is a pelvic floor specialist?
Doctors who specialize in pelvic floor dysfunction issues are called urogynecologists and physiotherapists. A urogynecologist will care for women with pelvic floor disorders by providing services that help evaluate pelvic floor health and provide primarily surgical treatments for pelvic organ prolapse. Their speciality covers the muscles, ligaments, connective tissues, and nerves within the uterus, vagina, bladder, and rectum.
A physiotherapist or Occupational therapist who specializes in pelvic floor treatment helps treat pelvic floor issues non-surgically. This is commonly done through exercise and manual therapy as well as extended education and advice on how to properly engage and strengthen your pelvic floor. Other specialists who aid in pelvic floor therapy include movement specialists and occupational therapists. Movement therapy can play a significant part in retraining the body toward correct posture, alignment, deep-tissue manipulation, and provide educational instruction on how the body works and how it heals.

What is involved in pelvic floor physical therapy?
Pelvic floor therapy most commonly involves exercises and education on how to properly engage and strengthen the pelvic floor. A specialist like a physiotherapist will help instruct their clients with a range of techniques ranging from:
- Breathing mechanics
- Therapeutic exercise & core building
- Pelvic floor realignment
- Proper posture
- Symptom treatment
- Physical education

Pelvic floor therapy seeks to instruct women in how their bodies work while also treating any conditions causing pain or embarrassing symptoms – like pelvic organ prolapse. When seeking treatment for pelvic floor dysfunction or POP, there are a few things you should keep in mind.
Professional Care
When seeking treatment for PFD or POP, make sure that the instructor or doctor is trained and educated in pelvic floor treatment. An initial assessment by a urogynecologist can assist you with a referral to a great physical therapy specialist.
Consultation
Seeking physical therapy for pelvic floor issues does not require a referral from a medical professional. When you see a physio, they will take a full history of your bladder and bowel function, sexual function and medical and surgical history. A pelvic floor assessment is commonly performed through what is called a manual palpation. This is an internal assessment to determine pelvic floor muscle function, strength, and overall health. They will also be interested in your fitness activities.
Treatment
Treatment for PFD could include exercises, biofeedback (electronic monitoring), and manual treatment of the muscles. In my programs I give extensive advice and education regarding daily activities and fitness, as well as good bladder and bowel habits, and proper posture and breathing mechanics. Function based training of the pelvic floor helps get your muscles back to working effectively when you need them.
RYC & Movement Therapy for PFD
In your search for pelvic floor therapy, you should consider a therapist trained in treating those with PFD – someone who is knowledgeable in their field and has experience in treating symptoms of PFD or POP. As an internationally recognized Yoga + Pilates teacher specializing in core and PF issues, I have been working with people for years with various core related issues. I am a longtime movement teacher with 20 years of experience guiding people through injury rehab. With my years of experience I have created online exercise programs that are challenging, unique, safe, sustainable, and life-changing for clients who may be facing difficult symptoms for PFD or diastasis recti such as prolapse, incontinence, chronic pain, and weakened rectus abdominis muscles.
When should you see a pelvic floor therapist?
Symptoms vary and differ from person to person. Whether your pelvic floor dysfunction is caused by an underlying illness or disease or caused by incorrect breathing mechanics or a result of an abdominal injury may also increase pain or play a part in the dysfunction of the pelvic region. Some of the most common symptoms associated with pelvic floor dysfunction may include:
- Urinary incontinence
- Rectal incontinence
- Incessant need to pee
- Difficulty in emptying your bladder or bowel
- A prolapse
- Pain in your pelvic region
- Painful sex
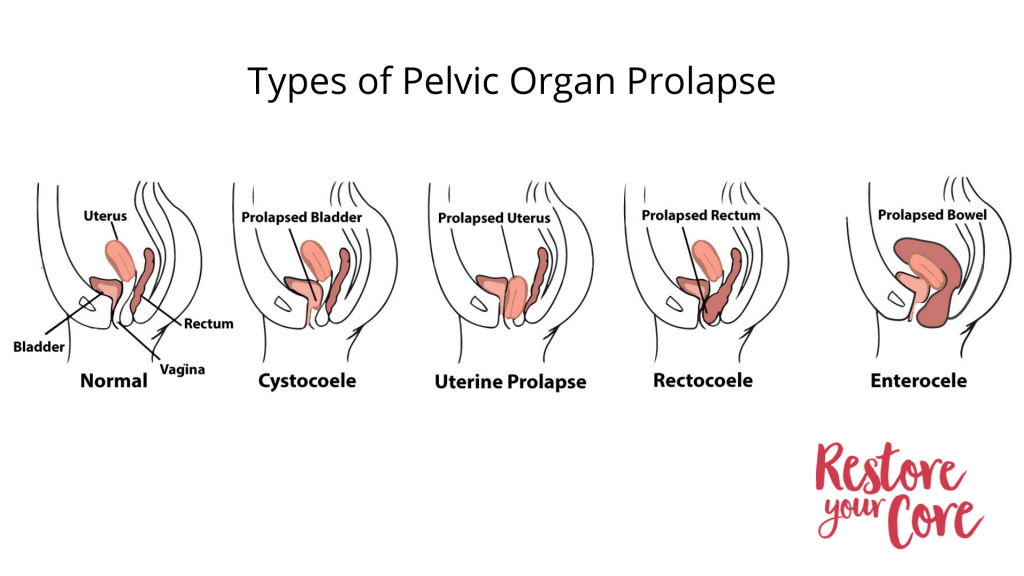
Tight and overused pelvic floor muscles can result in painful and embarrassing symptoms. Pelvic pain and loss of control with bowel movements can be an embarrassing result of pelvic floor dysfunction. If you are experiencing any of the symptoms above or any other discomfort or pain, you should consider contacting a medical professional to be assessed.
However, if these symptoms are present, there are ways to begin healing and loosen your pelvic floor muscles in order to gain back control over your body.
PF therapy can help
A physiotherapist will help increase muscular mobility and strength while helping reduce pain by teaching gentle stretches and exercises. They are specially trained to help strengthen or rehabilitate the pelvic floor. As you know by now, therapy goes way beyond kegels.
My 13 Week Program: Restore Your Core offers a step by step approach to strengthening your whole body. If you feel a bit unprepared to tackle a long program, here is a video of 5 exercises that are wonderful to get you started. Regardless of who you see and whether or not a medical professional is needed, PFD physical therapy can assist in treating painful symptoms such as:
- incontinence
- difficulty with bladder or bowel movements
- painful sex
- constipation
- pelvic pain
- endometriosis
- vaginismus
- menopause symptoms
- pregnancy and postpartum wellness
Article Source : restoreyourcore.com/pelvic-...